The Life Sciences Report: Can you elaborate on the costs associated with long-term care, which Moseda Technologies Inc. (MSD:TSX.V) can address?
Dr. Lisa Crossley: Chronic conditions account for over 75% of healthcare costs worldwide. These conditions are often poorly managed by patients at home, leading to complications and the need for emergency room (ER) visits, hospitalizations, long-term care facility admissions and other costly interventions. Readmissions cost the healthcare system precious funding, and U.S. hopitals are subject to payment penalties when a Medicare beneficiary is readmitted within a prescribed period with a complication that Medicare considers preventable. Approximately 20% of Medicare patients who are hospitalized end up back in the hospital within 30 days. Patient transport wastes precious healthcare dollars. In the U.S. each year, 2.2 million (2.2M) patients are transported between ERs to access the appropriate specialized care, at a cost of $1.39 billion ($1.39B). U.S. correctional facilities spend over $450M annually transporting inmates to ERs and doctors' offices. Assisted living facilities in the U.S. incur over $5B in transportation and medical costs associated with ER and physician office visits.
TLSR: We understand that Moseda is at the intersection of healthcare and technology. Please explain what this means, and describe the market opportunity in front of you.
LC: Over the last decade, there has been a dramatic increase in the development and adoption of information technology (IT) solutions for healthcare. From digital imaging to electronic medical records to consumer health apps, IT solutions have been developed to address the needs of health systems, clinicians, payors and patients. Healthcare IT solutions can improve health outcomes, reduce healthcare costs, enhance clinician and patient satisfaction, and increase access to care.
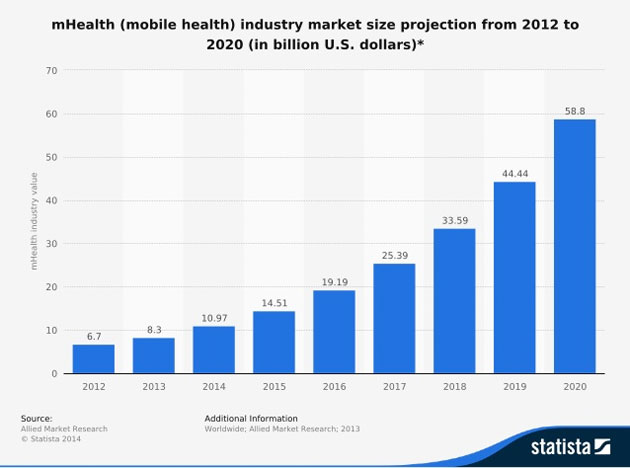
The global healthcare IT market grew from $99.6B in 2010 to $162B in 2015, at a compounded annual growth rate (CAGR) of 10.2%. Moseda is targeting the large and rapidly growing global market for community-based care, or virtual healthcare. According to BCC Research, this market reached $19.2B globally in 2014 and is expected to grow at a CAGR of 17.7%, exceeding $43B by 2019.
Moseda is targeting the large and rapidly growing global market for community-based care, which is expected to grow at a CAGR of 17.7%, exceeding $43B by 2019.
Support from governments worldwide in the form of stimulus packages has been a powerful driver in this market. Initiatives in Canada, the U.S., Europe, China and other jurisdictions to implement province-, state- or nationwide health records have fueled significant government investment in healthcare IT. In the private sector, a survey by industry research firm peer60 showed that the top priority for spending in 2015 for U.S. hospitals with greater than 250 beds was population health management, which can best be achieved through cost-effective high technology, low-touch solutions like Moseda's.
On the investment front, mobile health (mHealth) companies have received more than $3.5B in over 500 deals since 2010. In 2015 alone, over $1.3B in venture capital funding was invested in mHealth ventures.
TLSR: What makes Moseda's team suited to pursue the market opportunity?
LC: Our team has a strong track record of building and leading successful technology companies. Prior to joining Moseda, I was the CEO of three venture-backed companies, VitalHub, Quantum Dental Technologies and Natrix Separations. I've raised over $35M in venture capital and angel financing from major institutional investors and angel groups in the U.S. and Canada. I've had successful exits via M&A and IPO. I started my career running global therapeutics manufacturing for a biopharmaceutical company in Boston, and I've been in the healthcare space for over 20 years.
Our chief visionary officer, Giancarlo De Lio, is a healthcare IT pioneer who has developed multiple innovative mHealth products, and has founded and/or led numerous successful companies in the digital, healthcare, mobility and IT markets. Giancarlo founded and led CareKit Health, which Moseda recently acquired. Prior to CareKit, he founded VitalHub Corp., an mHealth company targeting the acute care enterprise market. Giancarlo is a serial entrepreneur who has had multiple successful exits via mergers and acquistions (M&A). He has a bachelor's degree in computer science and a master's degree in busines administration, so he's ideally positioned to evaluate trends in the mHealth marketplace and develop novel IT solutions that address significant unmet needs in major market segments.
Our Vice President of Products, Leo Godreault, is a registered nurse and entrepreneur with a strong background in information technology. Leo previously founded SmartMEDS, a healthcare IT company designed to improve the patient and clinician experience. Leo brings a unique combination of IT expertise and clinical experience to the CareKit Health team.
Leveraging the team's network and credibility in the healthcare space, Moseda has closely partnered with Microsoft Canada on the development and commercialization of the CareKit platform.
TLSR: Moseda recently acquired CareKit Health. How does this acquisition support Moseda's business strategy?
LC: Moseda is committed to developing and commercializing innovative mHealth and telemedicine solutions for community-based healthcare. We're excited to be bringing CareKit Health's technology, products and customer pipeline into Moseda. CareKit's focus on using technology to provide cost-effective, high-quality, in-home healthcare fits perfectly with Moseda's strategic focus on the community care market.
TLSR: Can you describe the CareKit Health platform?
LC: The CareKit Health platform is specifically designed to allow complex continuing care patients—patients with congestive heart failure (CHF), chronic obstructive pulmonary disease (COPD), diabetes, patients who need palliative care, and post-surgical patients—to receive high-quality care in the home. Moving the care of these patients from acute care centers to the community-based setting reduces costs, decreases the risk of hospital-acquired infections, provides patients with the comfort of a familiar environment and the support of their family and friends, and gives patients and families a sense of ownership and accountability for their own care.
The CareKit system consists of the CareKit app, a suite of "wearable" monitoring devices such as a pulse oximeter, glucose meter, activity tracker, spirometer, blood pressure cuff, scale, etc. (as appropriate to the patient's specific condition), and sensors and iBeacons to be placed around the patient's home. The system also includes a voice technology hub.
In the patient's home, CareKit uses the supplied wearables to collect patient health data. The sensors provide contextual reminders, and help visually or cognitively impaired patients with wayfinding. The interactive voice technology hub provides patients with audible alerts and reminders, along with voice-activated access to all of the information available through CareKit, including patient education materials, care team contact information, a summary of previously collected patient health data, and a current schedule of home visits, virtual consults, doctors' appointments and other upcoming interventions. CareKit Health empowers patients to actively participate in managing their own health at home.
TLSR: What are the key challenges in the community care market?
The CareKit system consists of the CareKit app, a suite of "wearable" monitoring devices, sensors and iBeacons placed around the patient's home, and a voice technology hub.
LC: As the population ages, global healthcare costs are rising significantly, and the existing healthcare business model is rapidly becoming unsustainable. Demand by governments, HMOs and patients for more efficient healthcare is driving healthcare organizations to reduce costs by moving care out of the acute, inpatient setting into the community. The key challenges in the community setting include poor access to specialized care in remote, rural and inner city settings and a shrinking percentage of healthcare personnel to care for more complex continuing-care patients. Chronic diseases account for 79% of all U.S. healthcare spending, but chronic conditions are often poorly managed by patients at home, leading to complications and the need for ER visits, hospitalizations, long-term care facility admissions and other costly interventions.
TLSR: What is the current standard of care for patients in the community?
LC: Currently, patients are monitored for risk of readmission and death by in-home care providers, where available, and by family, the patients themselves, primary care providers and specialized outpatient clinics—CHF, COPD, diabetes clinics—where they exist. This approach is not cost-effective, will be very difficult to scale as the population ages and, as shown by the literature, is not effective in reducing complications, ER visits or readmissions. Clinicians, families and patients are looking for a scalable, cost-effective solution that leverages technology to provide top-quality care in the community setting.
TLSR: How does post-discharge monitoring affect health outcomes?
LC: The current literature clearly shows that proactive monitoring of patients in their homes/community on a regular basis decreases repeat visits to the ER and readmissions. For example, for CHF patients post-discharge from hospital, the typical readmission rate at 20 days is 24%. But that can be reduced almost to zero with proactive and regular monitoring in the home. Self-reported quality of life for patients who are able to avoid hospital readmissions is likewise improved. Similar improvements in health outcomes have been demonstrated for COPD, palliative care, diabetes and post-surgical patients who receive proactive monitoring after discharge from hospital to the community.
TLSR: How do patients and families feel about using a system like CareKit?
LC: Studies consistently show that providing patients with chronic diseases and their families with a sense of ownership and accountability for their own care results in better health outcomes, which results in lower healthcare costs and helps improve the sustainability of the healthcare system. Patients and families consistently report increased satisfaction with quality of care when they feel that they are included as members of the patient's circle of care. CareKit was specifically designed for use by sick and elderly patients and by non-tech-savvy family caregivers. The system is highly intuitive and exceptionally easy to use.
TLSR: What differentiates CareKit from other remote patient monitoring solutions?
LC: CareKit's proprietary technology offers the only solution available today that comprehensively addresses the needs of complex continuing care patients, their families and the entire care team. CareKit Health's technology provides members of the circle of care with access to the patient's medical record, care plan and timeline (listing past and future home visits, virtual consults, physical appointments, procedures, etc.). The CareKit Health platform supports secure communication between all members of the care team as well as with the patient and family. This promotes collaboration among care team members; reduces the risk of redundant tests, procedures and home visits; helps ensure high-quality care in the home environment, with the corresponding low cost of care delivery; and increases patient and family satisfaction by keeping them in the loop. CareKit is also unique in its ability to integrate with hospital electronic medical record (EMR) and other clinical information systems, which supports the complete continuum of care from the acute setting to community physician practices to the home.
TLSR: Moseda is a Canadian company. Are you primarily targeting countries that have publicly funded healthcare like Canada?
LC: We're targeting both publicly and privately funded healthcare systems. Government-funded healthcare systems like those in Canada and the UK need to deliver efficient, cost-effective, high-quality care to the taxpayers who fund the system. Reducing the cost of care delivery to chronic disease patients who account for the vast majority of costs to the healthcare system helps ease the strain on these frequently overburdened systems, and ensures their sustainability in the future.
In the U.S., the largest privately funded healthcare system in the world, Medicare and Medicaid have started penalizing hospitals for patients who are readmitted within the first 30 days after discharge with what Medicare/Medicaid considers a "preventable complication." With CareKit Health, readmissions can be limited or avoided altogether, saving hospitals the significant penalty payments while also helping hospitals to attract new patients who want high-quality care in their home environments.
TLSR: When do you expect to have deployments of the CareKit system?
LC: We expect to launch pilot projects with hospitals in Canada and internationally in Q2/16 and also expect our first revenues from CareKit this quarter.
TLSR: Thank you for your time.
Dr. Lisa Crossley, CEO and director or Moseda Technologies Inc., is an accomplished healthcare technology executive with a proven track record of successfully building and leading global tech companies. She has diverse experience across multiple market segments, including healthcare information technology, therapeutics, medical devices, life science tools and diagnostics. Most recently, Dr. Crossley was CEO of VitalHub Corp., a healthcare IT company that provides clinicians with secure mobile access to comprehensive patient health information. Her prior experience includes leadership positions as CEO of Quantum Dental Technologies and President & CEO of Natrix Separations. Dr. Crossley has raised over $35M in venture capital and angel financing, negotiated channel partner agreements with major multinational market leaders, and built customer bases in North America, Europe and Asia. She holds a bachlor's degree in anatomy and cell biology from McGill University and a B.A.Sc. and Ph.D. in chemical engineering from Queen's University, and is a licensed professional engineer in the province of Ontario. Dr. Crossley currently serves on the Genome Alberta Board of Directors and on the Mitacs Research Council. She has previously acted as a board director for the Ontario Bioscience Innovation Organization (OBIO), Viron Therapeutics, Boyd Technologies, and Women in Science and Technology Businesses (WSTB), and has held numerous advisory board appointments. She was a member of the Council of Canadian Academies' Expert Panel commissioned by Industry Canada to conduct a comprehensive assessment of the State of Industrial R&D in Canada.
Chart courtesy of Moseda Technologies Corp.
Want to read more Life Sciences Report interviews like this? Sign up for our free e-newsletter, and you'll learn when new articles have been published. To see recent interviews with industry analysts and commentators, visit our Streetwise Interviews page.
DISCLOSURE:
1) Tracy Salcedo prepared this interview for Streetwise Reports LLC, publisher of The Gold Report, The Energy Report and The Life Sciences Report, and provides services to Streetwise Reports as an employee. She owns, or her family owns, shares of the company mentioned in this interview: None.
2) Moseda Technologies Corp. is a banner sponsor of Streetwise Reports.
3) Dr. Lisa Crossley had final approval of the content and is wholly responsible for the validity of the statements. Opinions expressed are the opinions of Dr. Crossley and not of Streetwise Reports or its officers.
4) The interview does not constitute investment advice. Each reader is encouraged to consult with his or her individual financial professional and any action a reader takes as a result of information presented here is his or her own responsibility. By opening this page, each reader accepts and agrees to Streetwise Reports' terms of use and full legal disclaimer.
5) From time to time, Streetwise Reports LLC and its directors, officers, employees or members of their families, as well as persons interviewed for articles and interviews on the site, may have a long or short position in securities mentioned. Directors, officers, employees or members of their families are prohibited from making purchases and/or sales of those securities in the open market or otherwise during the up-to-four-week interval from the time of the interview until after it publishes.